A Closer Look at Varicose Veins
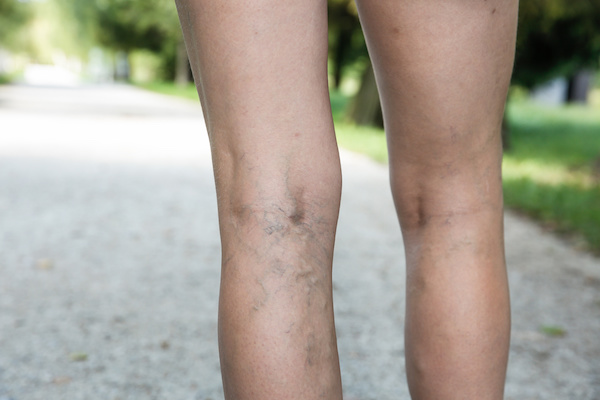
Varicose veins—visibly swollen, twisted veins under the skin—are very common, affecting nearly 25 percent of all adults. These blue- and dark purple-colored veins typically appear in the legs, but they can also develop in other areas, too.
Generally, varicose veins aren’t cause for concern. For many people living with them, they’re often a cosmetic issue or nuisance and not a health issue. However, there are times when varicose veins require treatment for health reasons.
Whether you’re considering treatment for your varicose veins for cosmetic reasons or health ones, it’s important to know more about them, including how they’re caused, diagnosed, treated and even prevented.
At Surgical Associates of Cleveland, we treat a number of patients each year for varicose veins, and our team often receives many of the same questions and concerns—some of which you may also have. We’ve got the answers!
Let’s take a look.
Causes of Varicose Veins and Who Is Most Likely Affected by Them
Simply put, varicose veins occur when the valves in your veins become weakened or damaged. When this happens, blood can back up and collect in the veins, causing them to swell up and twist.
Though experts are not certain why varicose veins happen, there are a number of known risk factors that increase the likelihood of developing them, including:
- being older
- having a family history of varicose veins
- leading an inactive lifestyle
- being female
- sustaining trauma to your leg or the area where the varicose vein appears
- being pregnant
- being overweight or obese
It’s important to note that while varicose veins are common, they typically do not cause medical issues. However, if varicose veins cause pain, blood clots, skin ulcers or other issues, a medical procedure may be necessary.
The good news, though, is that if treatment is necessary, it’s almost never invasive, and many options are simple, fast and easy to recover from.
How Varicose Veins Are Diagnosed and Treated
In most cases, a physician can diagnose varicose veins simply by physically examining them and asking patients about their symptoms (e.g., whether pain and/or aching is present in the affected area). Sometimes, further testing—such as an ultrasound to check for blood clots or malfunctioning valves—may be necessary.
Varicose vein treatment will depend on the severity of your varicose veins and the symptoms and/or complications they’re causing.
Your doctor may recommend making certain lifestyle changes if the varicose veins aren’t interfering with your health. On the other hand, however, if they’re leading to health problems, your doctor or surgeon may suggest having a procedure to either remove the varicose veins or close them.
Living with varicose veins: the power of practicing self-care
Self-care plays a leading role in managing and preventing varicose veins, as well as in your overall health.
Whether or not you need—or elect—to have a medical procedure to treat your varicose veins, you can help alleviate pain and pressure stemming from them, as well as prevent them from worsening, by:
- staying active—not only exercising, but also not standing or sitting for long periods of time
- maintaining a healthy weight
- not wearing tight-fitting clothing or high heels
- elevating your legs
Remember: You are your own best health advocate.
Are you living with varicose veins? To learn more about our treatment options for varicose veins or to schedule an appointment with one of our surgeons, call our office at (423) 472-5423.
